A gene editing medicine designed to treat two blood disorders has continued to perform strongly in clinical testing, with the latest results showing that, in the vast majority of treated patients, it alleviates the symptoms and burdens of both diseases.
Presented Saturday at a high-profile medical conference, the results represent another milestone for the therapy’s developers, Vertex Pharmaceuticals and CRISPR Therapeutics, which hope to ask for approval in the U.S., U.K. and Europe before the end of the year.
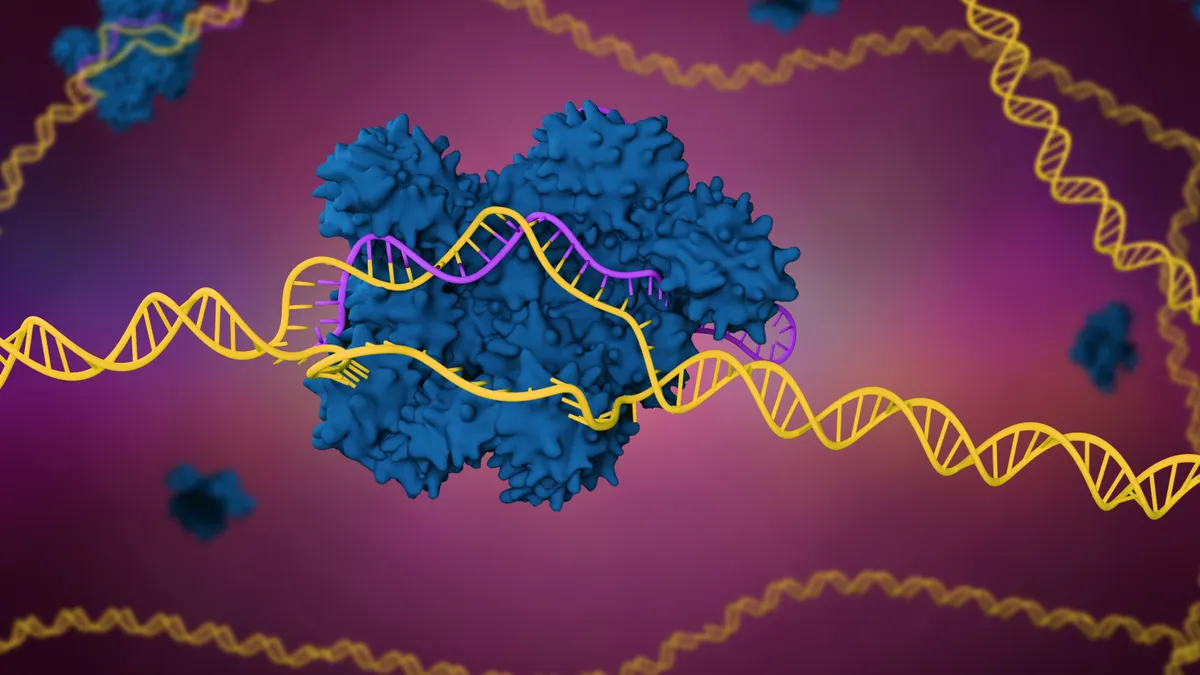
If approved, the therapy, now known as exa-cel, would become the first marketed medicine based on CRISPR, the landmark gene editing technology that won a Nobel Prize in 2020. It would also provide a new treatment option for patients with sickle cell disease or beta thalassemia.
While a small number of medications are cleared for use in these diseases, the only cure for them are stem cell transplants. The procedure is risky, though, and isn't available to many patients. Exa-cel may serve as another, perhaps more attainable fix, especially if Vertex and CRISPR can keep generating supportive evidence.
So far, the companies have released data on 75 treated patients, almost all of whom are now living without the most serious and impactful effects of their illnesses.
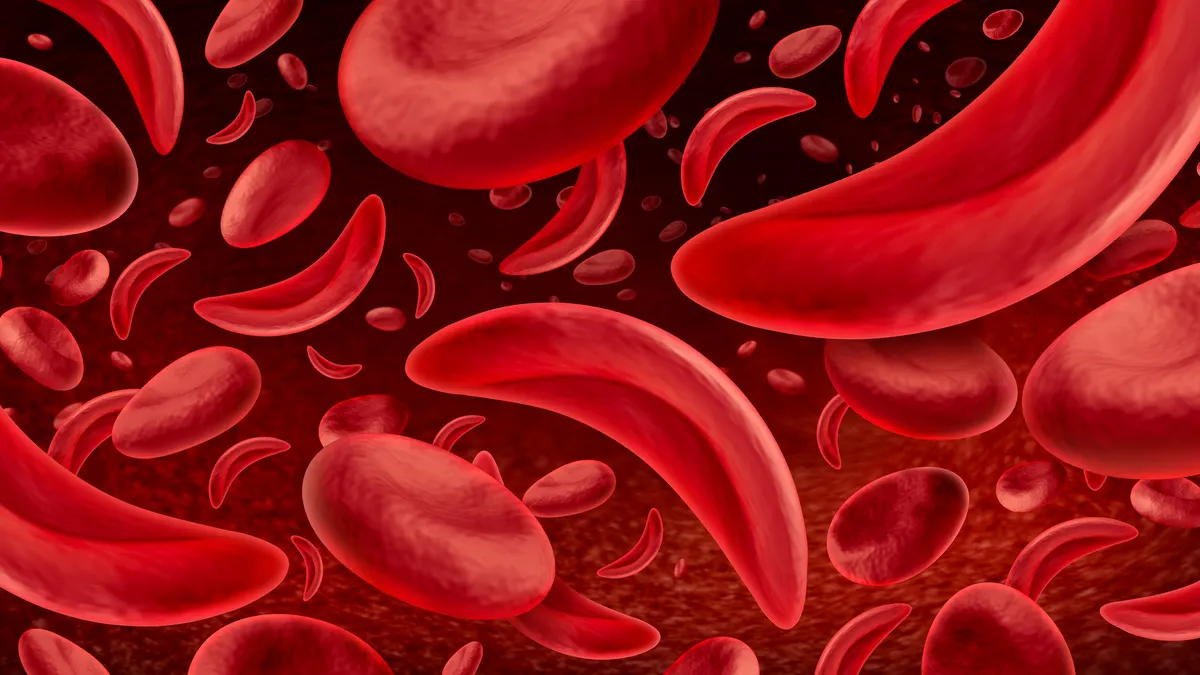
In sickle cell, genetic mutations give rise to misshapen red blood cells, which cause painful and sometimes life-threatening blockages known as vaso-occlusive crises. Beta thalassemia, meanwhile, is also an inherited condition, but one that hinders production of an oxygen-carrying protein called hemoglobin. In severe cases, patients require regular blood transfusions to survive, which can lead to the toxic buildup of iron in their organs.
The trial data presented Saturday are from 31 patients with sickle cell and 44 with beta thalassemia who are dependent on blood transfusions. In the two years leading up to the study’s start, the sickle cell patients experienced about four severe vaso-occlusive crises annually, whereas those with beta thalassemia received, on average, 36 units of red blood cells.
Since they were infused with exa-cel, none of the sickle cell patients have reported any crises, and all but two of the beta thalassemia patients have stopped transfusions. Transfusion volume did decrease in those remaining two patients, though, by 75% and 89%, respectively.
Notably, the amount of time trial participants have gone without these health issues varies. At the cutoff for data presentation, some had been followed for roughly three years, others only a month or two. It will therefore take more time for researchers to develop a complete picture of Vertex and CRISPR’s therapy.
Two beta thalassemia patients experienced so-called serious adverse events considered to be related to exa-cel treatment. Vertex and CRISPR previously reported one of those events, a potentially life-threatening immune reaction. Researchers are now saying that another patient showed low blood platelet counts and slower-than-expected engraftment of neutrophils — a type of while blood cell.
However, they noted that all of these serious adverse events resolved, and that none were seen in the sickle cell patients. No deaths have occurred and researchers haven’t detected any signs of cancer, a key concern for gene-based treatments.
To make their therapy, Vertex and CRISPR harvest stem cells from a patient, then genetically engineer them to reactivate a form of hemoglobin the body normally stops making after infancy. High levels of this protein have been associated with better outcomes for sickle cell and beta thalassemia patients.
For exa-cel to work, it must then be introduced back into the bone marrow. To do this, the patient is treated with a chemotherapy-based regimen meant to create space in the marrow for the engineered cells. But such regimens can be extremely difficult on patients. Prior results from the exa-cel trial found one patient, for example, experienced bleeding in the brain that researchers attributed to the precondition process.
While trial results continue to show promise, Vertex and CRISPR are changing how they measure treatment success, introducing new study goals for exa-cel in both sickle cell and beta thalassemia.
Before, the treatment’s goal was to reduce the transfusion burden for beta thalassemia patients and boost fetal hemoglobin levels for sickle cell patients. Now, it’s centered around independence from red blood cell transfusions and freedom from severe vaso-occlusive crises. A Vertex spokesperson said these adjustments “reflect the potential clinical impact of a one-time therapy like exa-cel.”
For Vertex, the successful development and approval of exa-cel could help offset recent setbacks in some of its other drug programs. While there are approved medicines for sickle cell and beta thalassemia, as well as logistical challenges ahead for a complex, outside-the-body treatment like exa-cel, the company appears confident in the commercial prospects for its therapy. This confidence was demonstrated last year, when Vertex agreed to pay CRISPR at least $900 million more for a larger cut of future sales.
Vertex and CRISPR aren’t the only drug developers to see an opportunity treating blood disorders with genetic medicines. Bluebird bio, Editas Medicine, and partners Sanofi and Sangamo Therapeutics, among others, are working on cellular and genetic therapies for sickle cell and beta thalassemia.
On Friday, advisers to the Food and Drug Administration unanimously endorsed Bluebird’s gene therapy for beta thalassemia, convinced by its powerful effect in freeing treated most patients from blood transfusions. The FDA is expected to make a decision on the therapy, called beti-cel, by August.