Editor's note: Second in an ongoing BioPharma Dive series on drug innovation. Above: Josh Hexter, chief operating officer of Oramed.
When it comes to innovation in the biopharma industry, the goal, according to the global consulting conglomerate Deloitte, is to “break the possibility frontier.” But what does that mean? And is that happening when drug companies apply the "innovative" label to products?
It's easy to say "no" to that latter question in many cases, especially in an era of "me-too" drugs that are so similar to products already on the market. But there are signs that this particular wave is slowing down.
According to Deloitte, drugs that break the possibility frontier “expand the range of possible outcomes while maintaining appropriate safety standards.” In short, innovative drugs are drugs that introduce a new mechanism of action (MOA), as well as drugs that treat diseases where there have historically been limited treatment options, such as orphan diseases, or drugs in a new therapeutic area where there has not been any progress for years.
'Me-too' drugs and the possibility frontier
To be clear, “me-too" drugs do not expand the possibility frontier, even if they are more convenient or have a slightly different formulation. Molecules that exert their effort via an already established MOA irrespective of advancement in the drug preparation are by definition not innovative.
Josh Hexter, chief operating officer of Oramed, a company that has developed an innovative technology to transform injectable treatments into oral therapies, says, “The era of ‘me-too’ drugs is on the downtrend.”
Citing the work of Ed Saltzman, the president of Defined Health, he says, “Proof of concept is no longer the threshold of measuring a drug’s value. Saltzman defines the new threshold as proof of relevance. That is to say the bar has been raised --- and raised significantly. It’s no longer just a question of, 'Does the drug work?' but 'How does it match up with other drugs/options?' ”
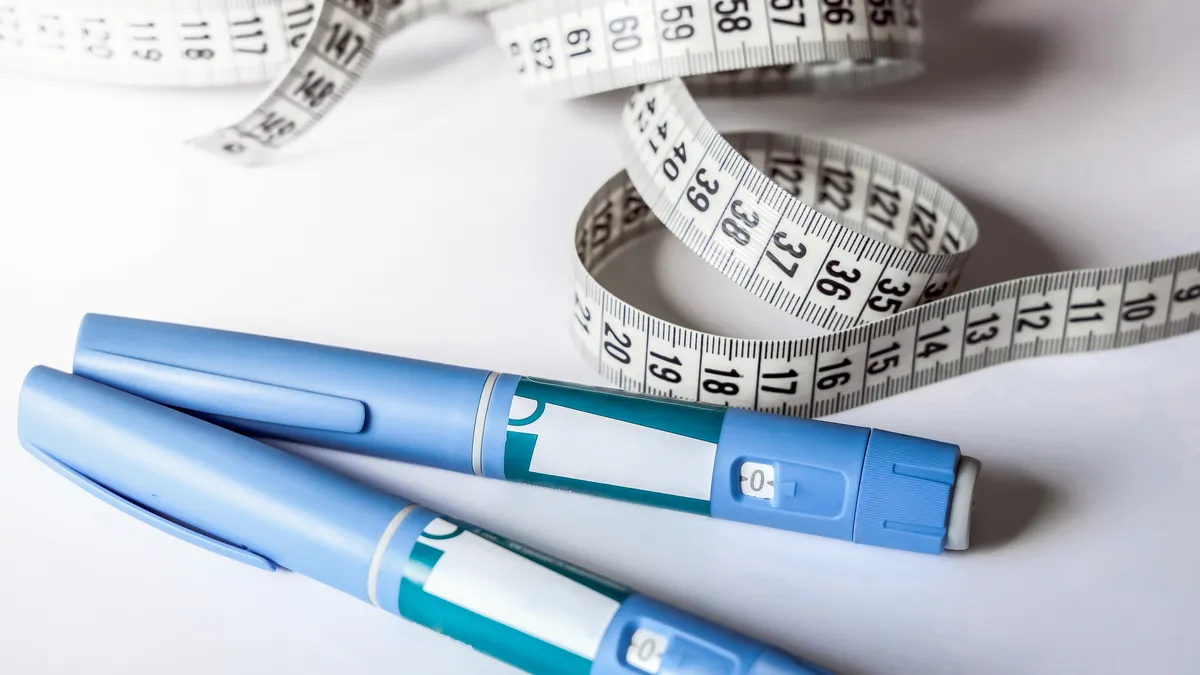
Recently, Hexter spoke to Biopharma Dive about why he believes his company’s oral insulin (ORMD-0181), currently in development, is truly innovative. It’s not just a question of a different delivery mechanism, but a new way to deliver a protein to the body, protect it and allow it to exert its therapeutic benefit. And because it’s oral and not injectable, it better mimics physiological insulin while avoiding the downside of needles.
Many recent 'innovative' drugs...aren't
When Deloitte conducted an analysis of 35 “innovative” approvals in 2011 (defined as new molecular entities (NMEs) or drugs that were granted priority review), it turned out that only seven of the 35 drugs met the criteria for being innovative. In fact, the analysts found that most of the NMEs from 2011 were using an established MOA and fell into the “me-too” drug bucket. Further analysis of the period from 2007 to 2011 showed that there were less than 10 innovative drug launches per year.
The three therapeutic areas where there is most likely to be a proliferation of “me-too” drug candidates are metabolic diseases, cardiology and infectious diseases. Although these drugs treat a very broad, and growing, population of individuals with chronic diseases, almost none of the drugs these categories break the possibility frontier, and overall the categories have become crowded.
Deloitte has highlighted three areas in which the highest level of innovation is occurring: orphan diseases, neuroscience and oncology. In fact, 75% of all cancer drugs approved in 2011 met the criteria for being considered innovative. One of the reasons why oncology has become so innovative as a category is because of the focus on personalized medicine in which molecular biomarkers are used to guide development, treatment and diagnosis of different types of tumors.
Hexter says, “The world of biomarkers has been exciting to watch. Biomarkers can help better show the mechanism of action of drugs and the push towards more patient-specific therapy. These biomarkers help better guide the pharma industry through clinical trials -- from patient selection to proof of concept. Also, the dovetailing of diagnostics and therapeutics in a commercial setting is yet another step closer to more personalized medicine. The confluence of innovation from both the world of pharma/biotech and the world of diagnostics is interesting and exciting.”
The excitement around biomarkers was palpable at BIO 2015, where Greg Daniels, managing director for evidence development and innovation at the Brookings Institution, led a panel discussion on biomarkers. By way of introduction, he defined the role of biomarkers as “critical in the emerging field of precision medicine.”
Toward that end, there are now more than 100 medicines with approved pharmacogenomics biomarkers in their labels, and the list is growing.
There was a time when Genentech’s Herceptin (trastuzumab), which was approved by the FDA in 1998, becoming the very first personalized medicine treatment option, was unique. However, the list is growing every month, including the recently approved Iressa (gefitinib), an oral treatment option from AstraZeneca approved for use in patients with locally advanced or metastatic EGFR mutation-positive non-small cell lung cancer (NSCLC).
In addition, Iressa comes with a companion diagnostic, co-developed by AZ and Qiagen. Iressa is precise, specific, targeted and---with an overall response rate of 70%---more effective in this patient population than other treatments. That’s called innovation.
The new reality of a payer-dominated world
In a world where payers are making stricter decisions and demanding value-based analyses to justify funding a drug, innovation is perhaps the surest way to have a drug accepted for widespread use. There are many ways to be innovative, but one would be to develop a drug to treat a condition for which there have not been any new treatments in years or even decades. Some examples of areas where there have been no approvals in the last 10 years include Lyme disease (where there are currently three development projects underway), testicular cancer (where there are four development projects underway) or toxoplasmosis (where there are two projects underway) -- just to name a few.
According to Hexter, in the final analysis, “The payer has become a demanding influencer in whether a drug will be a commercial success. Overall this is a good thing and it has pushed Big Pharma to look for innovation from biotechs and innovative companies who have pinpointed a need and developed a technological response. “