A gene therapy for bladder cancer that recently received $400 million in support from the private equity company Blackstone Group helped more than half of treated patients with resistant disease achieve remission.
The therapy, called nadofaragene firadenovec, was discovered by a Finnish-based research institute and first entered clinical study in 2012. The data revealed today at the Society of Urologic Oncology meeting came from a Phase 3 trial that is part of the agent's Biologics License Application now before the FDA.
Licensed by its original owner, FKD Therapies Oy, to Switzerland-based Ferring Pharmaceuticals, nadofaragene firadenovec is now in the hands of the U.S. subsidiary FerGene. That company was created with the Blackstone investment and an additonal $170 million from Ferring. FerGene will commercialize the gene therapy in the U.S., with Ferring holding rights elsewhere.
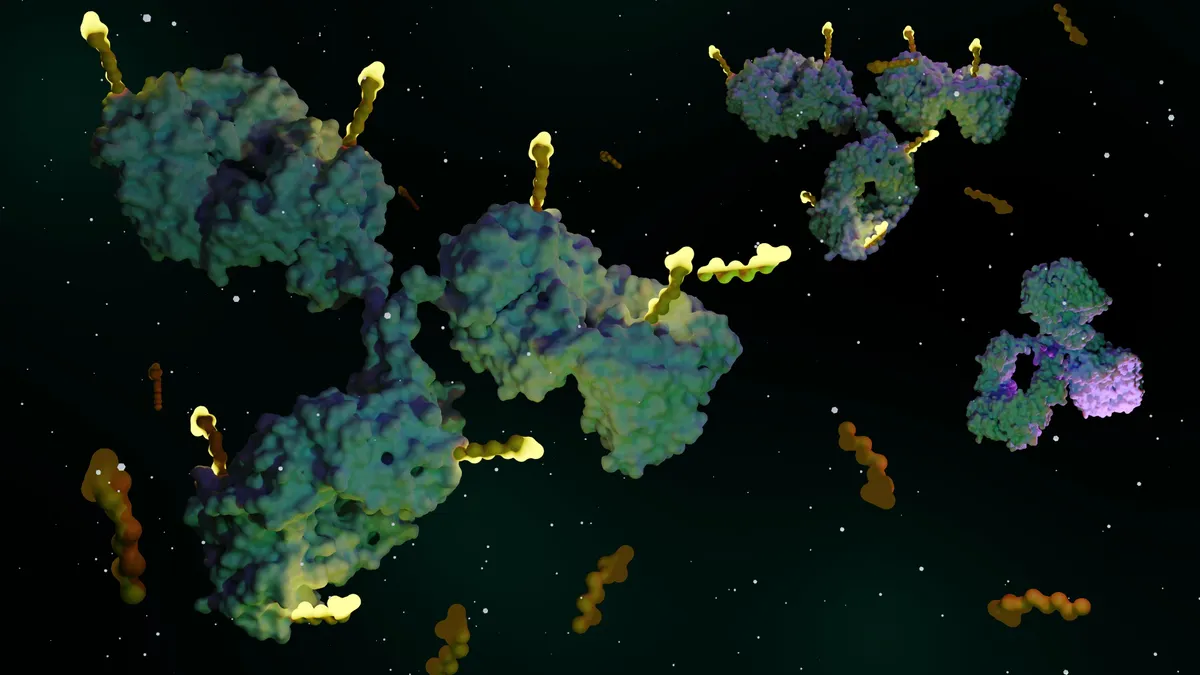
Nadofaragene firadenovec is an an adenovirus-based gene therapy encoding production of the immunity-stimulating protein interferon alfa-2b. Viral vectors containing the gene are administered by catheter once every three months into the bladder, where they are absorbed into cells in the organ's walls and begin stimulating interferon.
Delivery through a catheter, called intravesical administration, limits systemic exposure to both the viral vectors and to inteferon, said Neal Shore, medical director for the Carolina Urologic Research Center and an investigator in the trial. The side-effects of interferon include flu-like symptoms in patients who inject it for other conditions like multiple sclerosis.
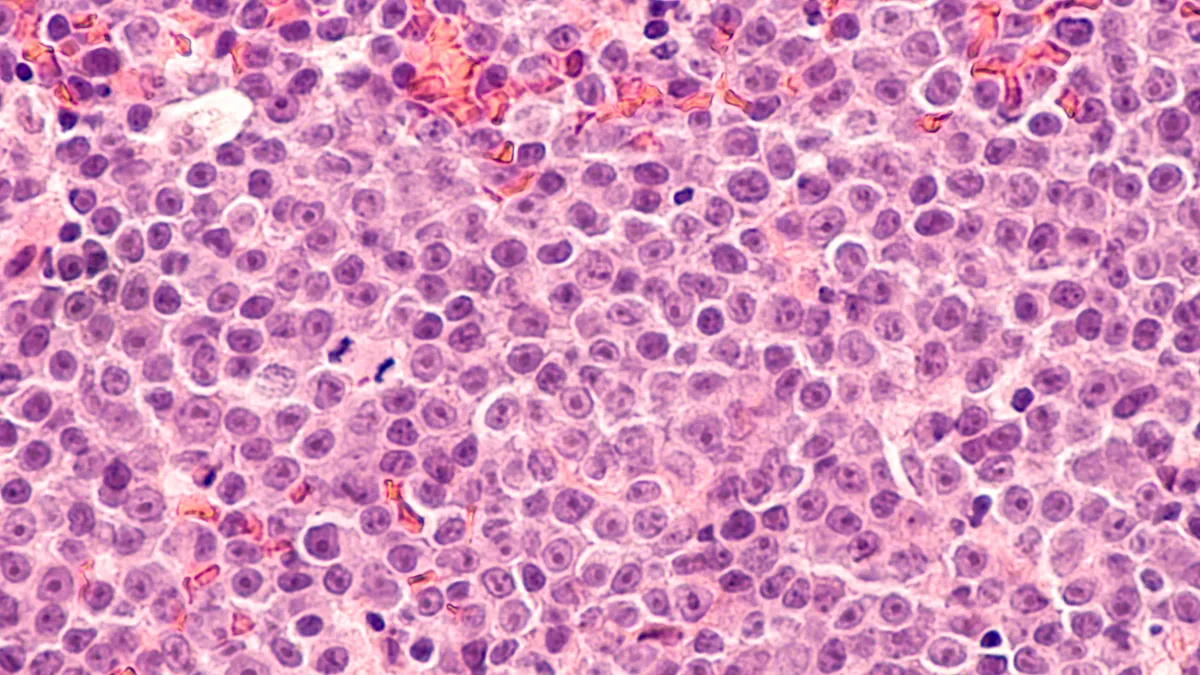
The clinical trial enrolled 157 patients with bladder cancer that has not spread to muscle walls and has stopped responding to treatment with Bacillus Calmette-Guérin vaccine.
Alternative treatments for these patients include chemotherapy or a procedure called "complete cystectomy." This surgery entails complete removal of the bladder, which in men means removal of the prostate and seminal vesicles and in women the uterus, ovaries, fallopian tube and part of the vagina.
"Radical cystectomy is one of the most invasive surgeries we do not just in urology but in all of surgery," Shore said, requiring a lengthy hospital stay and having a high rate of post-procedural complications.
Out of a group of 103 patients with superficial tumors in the bladder wall, just over half were in complete remission at three months, 41% at six months, and 24% at one year. In a group of 48 patients whose cancer had spread to the connective tissue outside the bladder, 73% had no recurrence of serious disease at three months, which fell to 44% at 12 months.
In this type of bladder cancer, the FDA has said a single-arm trial, without a placebo control, using complete remission is sufficient to be considered for approval, and the study does not need to pre-specify a rate that would define success. "The natural history of [disease] is well understood, and the complete response rate is negligible in the absence of therapy," the agency said in guidelines published in February 2018.
One chemotherapy agent, called Valstar (valrubicin), is approved for this patient group. It won FDA approval on a complete response rate of 18%.
In seeking FDA approval, nadofaragene firadenovec is in a race with Merck & Co.'s Keytruda (pembrolizumab) to achieve approval first. That immuno-oncology agent tested Keytruda in a similar population in the Keynote-057 trial, in which it achieved a 39% complete response rate.
Keytruda will be the subject of a meeting of the FDA's Oncologic Drugs Advisory Committee on Dec. 17.
Aside from the remission rates, Shore said nadofaragene firadenovec would differentiate itself from Keytruda in practice because its intravesical delivery means it could be administered by community-based urologists at outpatient clinics.