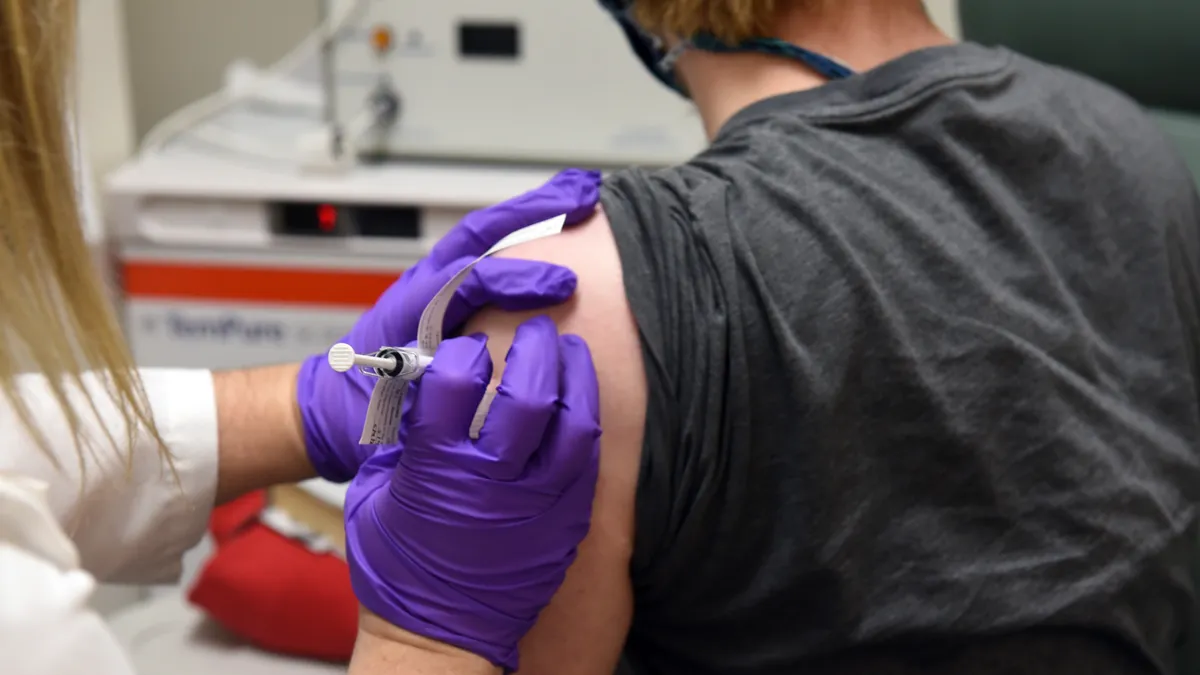
Within months, three massive trials in the U.S. could show whether a group of experimental coronavirus vaccines can prevent COVID-19. Even if all of them succeed, however, early supply of those shots will be limited, which is why it's fallen on public health authorities to figure out who will get access first.
The latest to weigh in on the issue is a committee from the National Academies of Sciences, Engineering, and Medicine, which on Tuesday published draft recommendations for the distribution of coronavirus vaccines.
Though several advisory groups and panels have made recommendations thus far, the committee's opinion carries significant weight because it will support the work being done by the Advisory Committee on Immunization Practices, or ACIP, which works with the Centers for Disease Control and Prevention. ACIP is currently developing a priority list that the U.S. may follow once a vaccine becomes available.
According to guidelines the National Academies committee posted Tuesday, healthcare workers and first responders, particularly those who have direct contact with COVID-19 patients, appear likely to be first in line. Workers in critical occupations and people who have medical conditions that make them particularly vulnerable to COVID-19 are also at the top of the list, followed, in succession, by broader groups who are at lower risk of contracting the disease or having serious complications.
Not all of them are likely to get access to a vaccine right away, however. Though vaccine developers have been ramping up manufacturing in tandem with advanced stage clinical trials — and taking on the risk that they will fail — the first batch of vaccines might only be large enough to immunize 10 to 15 million people, the National Academies panel wrote. Assembling a priority list, and backing that list up with clearly communicated rationale, will likely play an important role in earning public support for any immunization program.
In addition to the academy panel, ACIP, the World Health Organization and the Johns Hopkins University Center for Health Security have suggested healthcare workers be prioritized.
The difference between those recommendations is in terminology. ACIP, in past public meetings, has defined healthcare workers as a subset of essential workers, but has included people who aren't directly involved with patient care. The National Academies draft takes a narrower view, prioritizing those at high risk of acquiring infections.
This recommendation is a departure from the H1N1 influenza pandemic in 2009 and 2010. Because of how that disease affected different population groups, pregnant women and those with young babies, along with people under age 24, were prioritized ahead of older and sicker people.
In the National Academies draft framework, healthcare workers and first responders are part of the "jump start" phase, which would be followed by people with medical conditions that put them at higher risk of death or complication and then older adults in overcrowded living settings. The jump start phase would cover 5% of the U.S. population and the next stage would involve 15%.
The different frameworks all appear to agree that high-risk populations and essential workers are also close behind in the priority list, although there are some nuanced differences. The National Academies emphasizes the level of risk faced by employees who work in close quarters or can't telecommute, while the ACIP's framework, along with Johns Hopkins, focuses on roles essential to society. The National Academies draft does, however, highlight teachers and school staff as priority occupational roles.
The ACIP is due to meet again on Sept. 22. The U.S. government aims to have a coronavirus vaccine authorized for emergency use by later this year or early next.
Through the Trump administration's Operation Warp Speed, seven vaccine developers have received more than $11 billion in total funding from the U.S. Three — developed by Moderna, the team of Pfizer and BioNTech, and partners AstraZeneca and the University of Oxford — have advanced into large-scale efficacy trials that are expected to involve as many as 90,000 people. Other Phase 3 studies could begin this fall.